
In men, genital discharge from the urethra (urethra) and the secret of the preputial glands located on the head of the penis under the skin of the foreskin. The ejaculatory canal, prostate canals, urethra, and bulbourethral glands open into the urethra.
In a healthy person, only urine and ejaculate flow through the urethra. It is a physiological discharge from the penis and should not cause discomfort. Unfortunately, this is not always the case.
For a variety of reasons, men's health is shaken, and instead of normal flow, there is an abnormal flow or changes in urine and sperm.
Variants of physiological secretions
Criteria for normal excretion according to the functions of the organs of the urogenital system:
- Urine - clear, straw to golden yellow, practically odorless, free of flakes or other inclusions;
- The secret of the prostate has a viscous consistency and a whitish tinge, the sperm has a peculiar odor;
- Ejaculate: sperm from the ejaculatory canal are mixed with Littre's glands (urethral), Cooper's (bulbourethral) and prostate secretions to give a greyish-white color and a slimy texture;
- Fresh smegma from the subcutaneous glands is like a thick white fat; it may turn yellow or green over time.
The lubricant before the skin, the smegma, is constantly released, accumulating under the inner layer of the foreskin and in the coronal groove of the penis. The lubricant consists of fat and bacterial residues, is evenly distributed and reduces friction between the foreskin skin and the acorns. The maximal activity of the subcutaneous glands lies during puberty, the secretion decreases with age and stops completely in old age.
If personal hygiene rules are disregarded, smegma may accumulate under the folds of the foreskin. In this case, the fatty part of the lubricant oxidizes and the protein part decomposes (even rots) and the masses turn green, giving an unpleasant odor. The same process occurs in phimosis, when due to the fusion of the foreskin it is impossible to completely free the head of the penis from the skin folds and remove the smegma. Accumulation and breakdown of the lubricant can lead to chronic balanitis and balanoposthitis (inflammation of the foreskin and penis), increasing the risk of developing tumors.
Urethrorhoea, a slimy, colorless secretion from the bulbourethral and urethral glands. Discharge data are shown for men with excitement of libido. The purpose of selecting pure mucus is to lubricate the urethra and improve the passage of sperm. The amount of secretion ranges from low to abundant, and these parameters are related to the individual characteristics of the body and the frequency of sexual activity. After prolonged abstinence, the amount of secretion increases.
Contamination is the spontaneous release of sperm that is not related to intercourse. It is usually seen in the morning when testosterone levels rise. It depends on age and the intensity of sexual activity: it occurs in puberty in boys and irregular or infrequent intercourse in adult men.
Prostatorrhea, a small amount of transparent mucus from the urethra with off-white inclusions. Occurs after tension in the abdominal muscles (such as constipation) or urination. The secret consists of a mixture of sperm and prostate secretions, and an increase in volume and transparency may be a sign of prostatitis.
Pathological discharge
In men, discharge from the penis can be caused by STDs, tumors, non-specific inflammation of the urogenital organs, various injuries, medical manipulations, or surgeries.
Abnormal urethral discharge is normal:
- By volume (too abundant or low, possibly moderate);
- In color and transparency (white to yellowish green, cloudy);
- By impurities (blood, pus, lumps);
- Consistency (very thin or too thick and sticky);
- By smell (sour, rotting, fish);
- According to the frequency of occurrence (depending on the time of day, permanent or episodic discharge);
- Regarding urination, sexual arousal, alcohol consumption, consumption of spicy and spicy foods.
The nature of the secretion depends on the pathogen of the disease, the condition of the immune system, the comorbidities, and the severity and duration of the inflammation (acute or chronic).
If the amount, density, color of the secretion changes, an unpleasant odor occurs, it is recommended to consult a doctor and perform tests. Self-diagnosis is not worth it, it is very difficult to correctly recognize the disease based on just one symptom.
Secretions from the penis associated with STDs
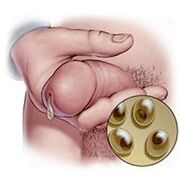
Mucosa: Clear secretions, viscous and found in small amounts in chronic chlamydia, mycoplasma or ureaplasma urethritis. Microscopic examination reveals a moderate number of leukocytes in the secretions (the norm is up to 4 cells per field of view).
Mucous membranes: white flow, translucent; observed in the exacerbation phase in chlamydia, ureaplasmosis, and mycoplasmosis. During chlamydia infections, they accumulate on the head of the penis as if they were "sticking" to the skin.
In the pathologies described above, the secretions come from the urethra itself, as the microorganisms irritate the mucous membranes of the urethra and the body tries to "wash away" it.
Sometimes the secret of white seems to cover your head. This is observed in chlamydia, candidiasis. In the first case a film is formed, in the second a loose cheese bloom.
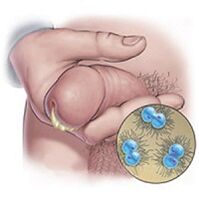
Purulent discharge with an unpleasant odor is characteristic of gonorrhea. Sticky, thick, yellow or greenish in color, with a rotting odor. Microscopic examination of the substance shows epithelial cells from the urethra, many leukocytes.
Symptoms associated with gonorrheal urethritis: persistent and copious discharge; the pain, itching and burning sensation are particularly strong during urination.
Sexually transmitted diseases are often associated with combined infections that combine several pathogens at the same time. Gonorrhea and trichomoniasis are accompanied by chlamydia, and mycoplasmosis and ureaplasmosis usually occur in pairs. The symptoms of such diseases are different from the classical manifestations, and urethral discharge may be of a completely different nature. Therefore, modern analytical techniques are used for the final diagnosis with high reliability rather than discharge characteristics.
Non-specific (non-sexually transmitted) inflammation
The cause of non-specific inflammation is its own microflora, which is conditionally pathogenic and is activated only in the case of problems related to the body's immune defenses. Streptococci and fungi belonging to the genera Staphylococcus, Candida and E. coli are always present on the skin surface and mucous membranes, but after hypothermia, prolonged stress, uncontrolled antibiotic treatment, radiation begins to actively multiply and displace beneficial bacteria. and chemotherapy.
Non-gonorrhea (non-specific) urethritis. Inflammatory secretions are small volumes in the form of mucosal cords or nodules visible in the urine at the very beginning of the disease. Burning and itching symptoms during urination are less pronounced than in gonorrhea, but urge is common and does not bring relief. In the case of an ascending infection, the bladder first becomes inflamed and then the ureters and kidneys; discharge appears with a scarlet mixture.
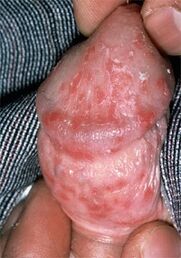
Candidiasis, a fungal infection of the urethra. It is usually caused by the suppression of the immune system after antibiotics, chemotherapy or radiation therapy; sexual transmission of candidiasis is rare in men. Thrush is characterized by a flow of clots with a sour smell, which is accompanied by itching and a burning sensation during urination (urination) and ejaculation (ejaculation), and may be accompanied by dull pain in the groin, above the pubic area and lower back.
Tendonitis of the urethra. The fishy odor of the secretion is characteristic; slight, yellowish-white or greenish. According to some classifications, gardnerellosis is called STD, but in men, sexual infection with gardnerella is more interesting. In fact, this disease is associated with a violation of the normal microflora, i. e. , dysbiosis. Immune correctors and probiotics (lactic acid bacteria) are necessarily used in its treatment.
Balanoposthitis, an inflammation of the foreskin. Abundant purulent discharge is observed locally, mucus mixing is possible. It is always accompanied by edema and hyperemia (redness) in the leaves of the prepuc, as well as pain in the head of the penis.
In case of prostatitis, cloudy discharge appears at the end of urination, copious discharge - in the acute period of inflammation; few and white - with the transition of the disease to a chronic form. Prostatitis is usually complicated by difficulty urinating and a poor erection, in severe cases up to anuria (complete lack of urine flow) and impotence.
Excretion is not associated with inflammation

Spermatorrhoea - secretion in the form of passively flowing sperm, without sexual intercourse or self-satisfaction, without feeling orgasm. The causes are certain nervous system diseases, spinal cord injuries, chronic stress and any prolonged inflammation of the genitals. Sperm are associated with impaired innervation and decreased iron deferens tone.
Hematorrhoea, spotting. It often appears when the urethra is damaged during a bougienage, after inserting a catheter, or after taking a mucosal smear. In these cases, the blood is fresh, blood-free, the volume is small, and the bleeding stops quickly. If small kidney stones or sand leave, blood is released during or immediately after urination, the bleeding is accompanied by very severe pain (kidney colic). In the haematological form of glomerulonephritis (inflammation of the glomeruli of the kidneys), the emptying of the blood is combined with edema and persistently high blood pressure, with the appearance of protein in the urine.
In the case of malignancies of the prostate, urethra or bladder, the discharge is brown, with blood clots or mucous membranes, a mixture of pus. Brownish mucus may form during the healing of wounds on the mucosa and is excreted by polyposis of the urethra and / or bladder.
Prostate rhea is the secretion of the prostate gland that flows out of the urethra. It occurs in chronic prostatitis, prostate adenoma, damaged nerve (neurogenic bladder).
Examination algorithm for pathological secretion of the penis
- Examination of the dam, penis, foreskin and acorns. The goal is to prevent genital deformities, signs of injury, signs of external inflammation, discharge, rashes, and so on. identification. Traces of discharge are sometimes noticeable on the bedding.
- Feeling of the groin lymph nodes, assessing their condition: size, warmer or colder than the surrounding tissues, painful or not, soft or dense, agile or clinging to the skin, if there is an ulcer.
- Finger examination of the prostate; massaging the prostate through the rectum and recovering secretions for microscopic examination. It is advisable to refrain from urinating for 1-2 hours before the massage. In prostate adenoma, the lobes are roughly enlarged and dense fibers can be felt. In the case of a malignant tumor, uneven growths and their consistency are typical, and blood clots can be released from the urethra when the prostate is palpated.
- Materials - smears for microscopy and culture. Examined under a microscope, the stained smear shows blood cells, epithelium, sperm, fat inclusions, and some pathogens (Escherichia coli, gonococci, gardnerella, yeasts). Increased leukocyte counts are characteristic of acute urethritis or exacerbation of chronic inflammation, eosinophils - allergic urethritis. Erythrocytes are found in severe inflammation, tumors, urinary tract injuries, urolithiasis. A large amount of epithelium is a sign of chronic urethritis, the urethral leukoplakia. In the case of spermatorrhea, the sperm cells are found in smears, in the case of urethhorrhoea - mucus, prostatorrhea - in lipid particles. To ensure the content of the information and the reliability of the results, the smear should be taken no earlier than 3 days after topical application of antibiotics, antifungals and disinfectants. If antibiotic treatment has been systemic, at least 3 weeks should elapse after treatment. Do not wash before taking a smear, try not to urinate for 2-3 hours.
- General clinical analysis of blood, blood glucose - in the morning, on an empty stomach. Extended urine test (morning dose, immediately after sleep).
- Ultrasound of the prostate, bladder and kidneys; CT and urography.
If the genital inflammation is severe, the patient will be prescribed a broad-spectrum antibiotic immediately before obtaining the test results. Excessive bleeding requires hospitalization and active bleeding. Confirmation of the suspicion of a malignancy can only be the result of a biopsy, the final diagnosis being made on the basis of histological examination.
Important:
- Penile discharge is just one symptom that cannot be considered when making a diagnosis.
- The independent appointment of the economy is unacceptable. drugs, even if the manifestations appear obvious for a particular disease.

























